TBI - Traumatic Brain Injury Overview
 TBI is an acronym for traumatic brain injury. A TBI is caused by head injuries from an external cause/force that damage the brain. The word 'traumatic' refers to the physical injury itself, not emotional trauma or severity level. A traumatic brain injury is also an acquired brain injury or ABI (an injury that happened after birth).
TBI is an acronym for traumatic brain injury. A TBI is caused by head injuries from an external cause/force that damage the brain. The word 'traumatic' refers to the physical injury itself, not emotional trauma or severity level. A traumatic brain injury is also an acquired brain injury or ABI (an injury that happened after birth).
How TBIs Happen
Many things can cause TBIs and they are usually sudden and swift. Physical assaults, domestic and child abuse, vehicle accidents, blast waves, falls, gun injuries, suicide attempts, and sports are common causes of TBIs. Millions of people every year experience a TBI but the majority are not severe.
Who Receives TBIs
Males are twice as likely to receive a TBI than females. This may be because males engage in more high risk activities, extreme sports, and receive industrial injuries at a higher rate. Riding a motorcycle, even with a helmet, is a leading cause of TBI. If you want to reduce your risk of a brain injury, avoiding motorcycles is a great choice.
Infants are especially vulnerable to brain injury because the fontanelle or "soft spot" in the skull will not close until the child is between eight to fifteen months old.
Every person is at risk for TBI. But it is possible to limit your risk of TBI by taking common sense lifestyle steps.
 What Occurs
What Occurs
TBIs happen when the head or neck comes into contact with something and the force of impact causes injury to the brain.
These may be a 'focal' injury (one that's localized) or a 'diffuse' injury covering a larger area. Injury types may be closed head - no visible damage - or involve an object that penetrated the skull and damaged the outer layer of the brain.
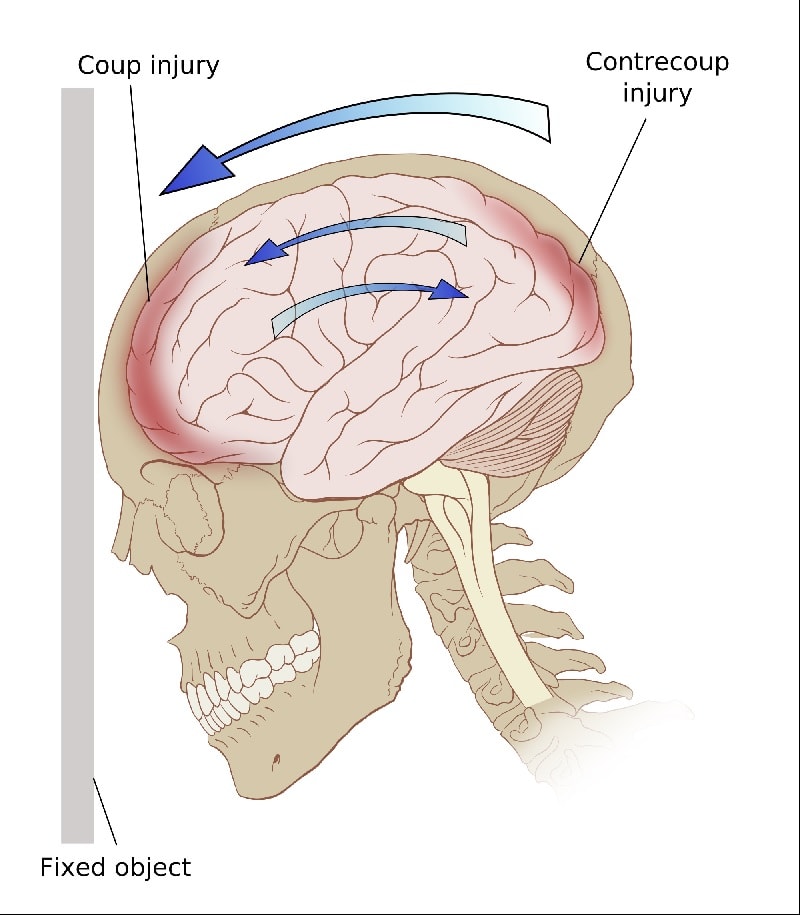
Coup and contrecoup traumatic brain injuries may happen separately or together. Coup injuries happen at the place of impact; the contrecoup injury is the opposite side of the head. Contrecoup injuries are typical when the force of a hit slams the brain into the skull.
 TBI Injury Levels
TBI Injury Levels
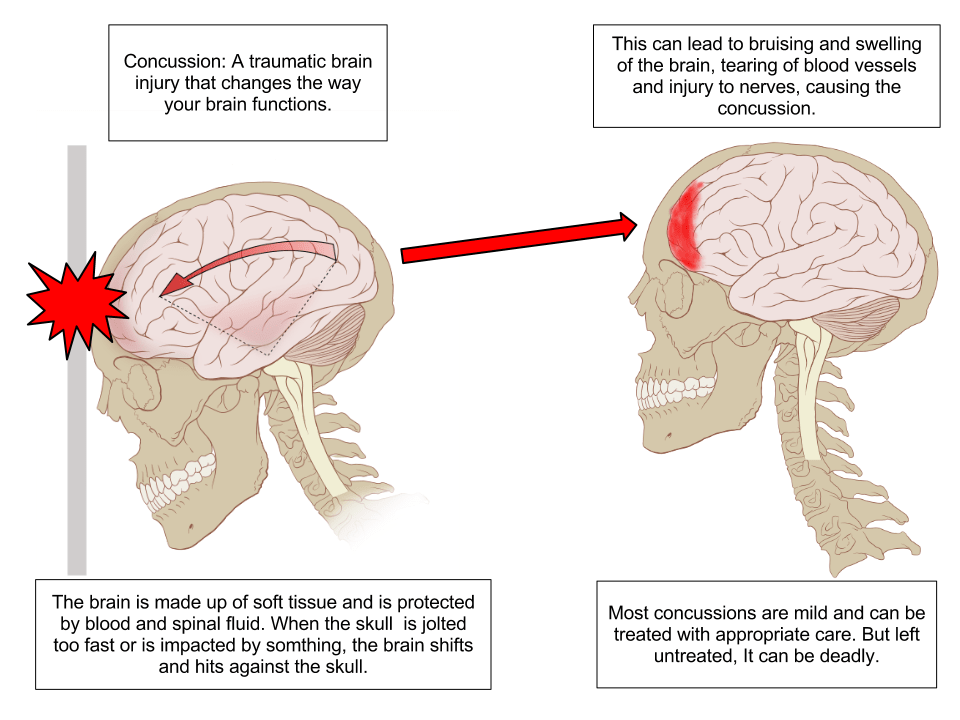
TBIs are classed as mild (like concussions shown at right), moderate or severe.
A medical professional who treats the injured person will use the Glasgow Coma Scale to identify the person's level of consciousness.
The injury is ranked in severity based on the person's eye, motor and verbal responses. The scale runs from 3 - 15, with lower numbers connoting more serious trauma. A GCS score of 8 or below indicates a severe TBI. This person would typically be in a coma or very altered state.
TBI Location Affects Function
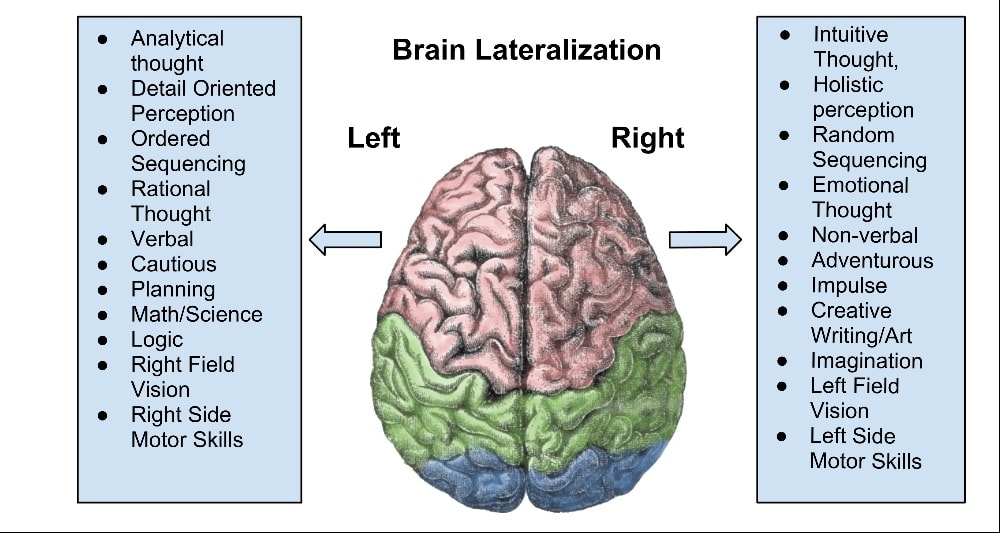
The location of the injury has a large influence on what functions of the brain may be impacted. The side of the brain, the lobe area, all matter. A few inches can determine whether short term memory is affected, whether speech is affected, etc. The type of brain injury - diffuse or focal - will implicate different areas of the brain and functioning as well.
First Response
The initial medical people on the scene will stabilize the person for transport to a hospital if the injury needs immediate care or further evaluation. They will use the Glasgow scale and treat external wounds. A person with suspected TBI will be taken to the emergency room for trauma care.
Hospital
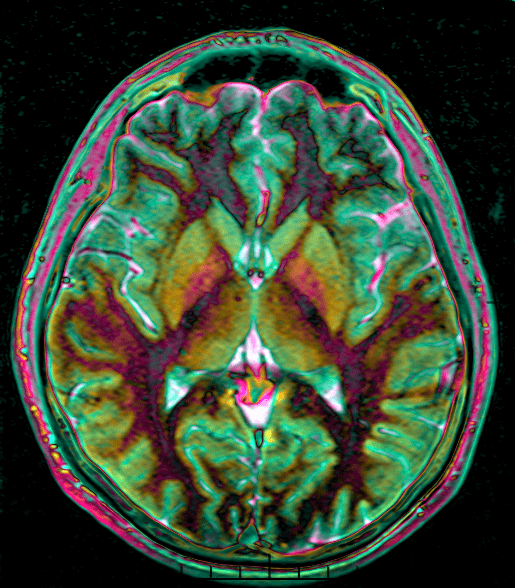
At the hospital, brain imaging studies will be done such as MRI or CT scan to look at the brain itself and inspect the injury location for any type of damage.
Even a mild TBI such as a concussion can have potentially dangerous effects if there is bleeding in the brain that goes untreated. It's a safety precaution to review any head injury for unexpected issues.
Some damage to the brain may not be visible in imaging, especially with concussions. It's not unusual for someone with a concussion to "shake it off" but experience later symptoms with mental processing.
After imaging review the person will be admitted to the hospital if necessary for surgery, intensive care or observation.
When families arrive at the hospital, they will have many questions but the nature of TBI doesn't lend itself to immediate answers. TBI can be a fast-changing situation and even under the best conditions the full extent of deficits may only emerge over time. Doctors are typically unable to predict how a loved one's condition may change or improve in the first days after brain injury.
Intensive Care for TBI
Life threatening injuries from TBI receive round the clock care in the intensive care unit. If none is available at the hospital, a person may be airlifted to a trauma center nearby that is better equipped. An intensive care unit (ICU) may also be called a critical care unit (CCU) or intensive treatment unit (ITU).
Depending on the extent of injuries, families may not be able to see their loved one for a period of time. There may also be restrictions on visitation time or gown requirements. The patient's condition may be described in various ways, such as "good," "fair," "serious," or "critical," but these are not really medical terms. According to the Maryland Hospital Association Handbook, the general meanings are:
*Good: Vital signs such as pulse, temperature and blood pressure are stable and within normal limits. The patient is conscious and comfortable. Outlook for recovery is good or excellent.
*Fair (also satisfactory or stable): Vital signs are stable and within normal limits. The patient is conscious, but s/he is uncomfortable or may have minor complications. His outlook is favorable.
* Serious (also poor or guarded): The patient is acutely ill with questionable outlook. Vital signs may be unstable or not within normal limits. A chance for improved outlook.
* Critical: Questionable outlook. Vital signs are unstable or not within normal limits. There are major complications. Death may be imminent."
Acute Rehab
Once a patient's condition improves, the hospital will begin rehabilitation. This may include physical rehabilitation for motion, balance, strength and mobility; speech language therapy; and cognitive therapy for difficulties with memory and other mental processing. When the TBI patient is ready to be discharged, they typically continue rehabilitation at a post-acute facility outside of the hospital.
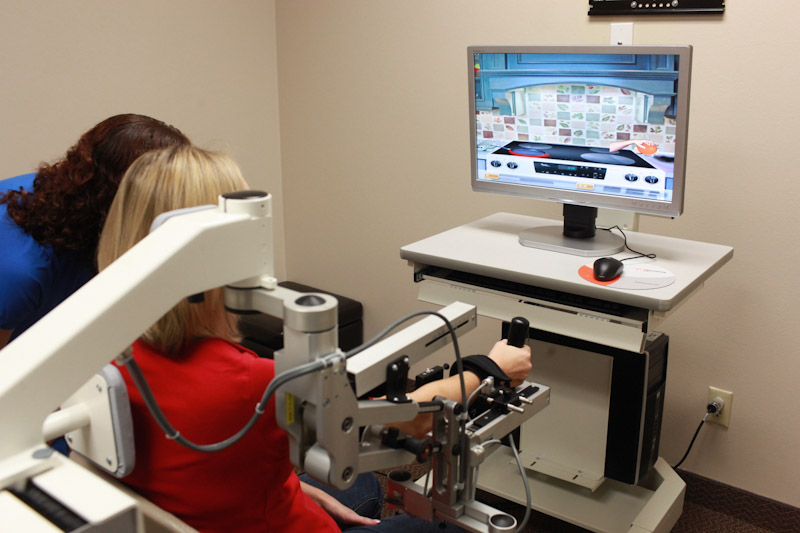
Post Acute TBI Rehabilitation
At this point, a person with TBI leaves the hospital and can begin their long term recovery. The challenges for people with traumatic brain injury are complicated.
Because the brain controls everything in the body, a brain injury can affect physical and mental abilities, as well as emotions. Comprehensive, multi-disciplinary rehab is recommended to allow the person with a TBI to reach his or her full potential for independence.
It is true that the level of injury is a factor in how much function can be regained but it is not the only determining factor. People with the most severe injuries can and do recover to return to their lives. The most important thing to remember when considering outcome is that every person and every traumatic brain injury is unique. A broken bone is going to heal pretty much the same way for people. A TBI is quite different.
